TMJ Disorder Treatment in North Miami

Treating TMD with physical therapy is an effective method to relieve pain and discomfort. When you come to Integrated Physical Therapy in North Miami, Aventura, and Wynwood for your evaluation and TMJ pain treatment, you can expect your therapist to analyze your jaw mobility and release muscle tension in the head and neck region. Our physical therapy team specializes in TMJ disorder therapy and is Mariano Rocabado Trained. We will perform a comprehensive evaluation of your TMD, neck, thoracic spine, and shoulder girdle to determine the structures causing TMJ symptoms.
Our patients are receiving immediate relief with our specialized TMJ physical therapy. Here is what they are saying:
“My pain is under control thanks to IPT. I only regret I didn’t come earlier." - A. S.
“I didn’t know physical therapy could help me with my jaw pain but after only a few visits, I was pain-free. Unbelievable!" - S. W.
“The team did an amazing job helping with my pain and chronic discomfort and I can’t thank them enough” – A. G.
What are the temporomandibular joints (TMJ)?
Simply stated, the temporomandibular joints (TMJ) are the two joints that connect your jaw to your skull. More specifically, they are the joints that slide and rotate in front of each ear, and consist of the mandible (the lower jaw) and the temporal bone (the side and base of the skull). According to the American Dental Association (ADA), the TMJs are among the most complex joints in the body. These joints, along with several muscles, allow the mandible to move up and down, side to side, and forward and back. When the mandible and the joints are properly aligned, smooth muscle actions, such as chewing, talking, yawning, and swallowing, can take place. When these structures (muscles, ligaments, jaw bone, mandible, TMJ) are not aligned, nor synchronized in movement, several problems may occur, requiring TMJ pain treatment in North Miami, Aventura, and Wynwood.
What is temporomandibular disorder (TMD)?
Temporomandibular disorders (TMD) are disorders of the jaw muscles, temporomandibular joints, and/or the nerves associated with chronic facial pain. Any problem that prevents the complex system of muscles, bones, and joints from working together in harmony may result in temporomandibular disorder, which can be effectively treated with TMJ physical therapy.
The National Institute of Dental and Craniofacial Research, part of the National Institutes of Health (NIH), classifies the categories of TMD by the following criteria:
Myofascial pain, the most common form of TMD, which is discomfort or pain in the muscles that control jaw function and the neck and shoulder muscles. This can be addressed through TMJ disorder therapy.
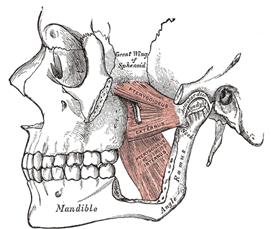
Internal derangement of the joint. This means a dislocated jaw or displaced disc, or injury to the condyle (the rounded edges of the jaw). TMJ physical therapy can help with this condition.
Degenerative joint disease, such as osteoporosis or rheumatoid arthritis in the jaw joint. TMJ pain treatment in North Miami, Aventura and Wynwood can provide relief for these conditions.
Most oral health professionals will agree that the primary cause of this disorder is excessive strain on the muscle group that controls chewing, swallowing, and speech. This strain may be a result of bruxism (incessant clenching of the teeth), or from physical or mental stress. These factors may be the cause, in most cases, or may aggravate an existing condition of TMD, which can be managed through TMJ disorder therapy.
What are the symptoms of TMD?
The following are the most common symptoms of TMD that can be addressed with TMJ physical therapy in North Miami, Aventura and Wynwood. However, each individual may experience symptoms differently. Symptoms may include:
- Jaw discomfort or soreness (often most prevalent in the morning or late afternoon)
- Headaches
- Pain radiating behind the eyes, in the face, shoulder, neck, and/or back
- Earaches or ringing in the ears (not caused by an infection of the inner ear canal)
- Clicking or popping of the jaw
- Locking of the jaw
- Mouth motions are limited
- Clenching or grinding of the teeth
- Dizziness
- Sensitivity of the teeth without the presence of an oral health disease
- Numbness or tingling sensation in the fingers
- A change in the way the upper and lower teeth fit together
The symptoms of TMD may resemble other conditions or medical problems. Consult a dentist, physician, or TMJ physical therapy specialist in North Miami, Aventura and Wynwood for a diagnosis.
What are the treatments for TMD?
Specific treatment for TMD will be determined by your physician, dentist or physical therapist based on:
- Your age, overall health, and medical history
- Extent of the disease
- Your tolerance for specific medications, procedures, or therapies
- Expectations for the course of the disease
- Your opinion or preference
Treatments include:
- Physical Therapy
- Resting the temporomandibular joint (TMJ)
- Medication and/or pain relievers
- Relaxation techniques and stress management
- Behavior modification (to reduce or eliminate the clenching of the teeth)
- An orthopedic appliance or mouthguard worn in the mouth (to reduce bruxism)
- Posture training
- Diet modification (to rest the jaw muscles)
- Specialized Therapy
Don't let TMJ pain control your life any longer. At Integrated Physical Therapy & Wellness, our team is ready to help you find relief through specialized TMJ physical therapy and treatment. We offer personalized care tailored to your unique needs, helping you regain comfort and improve your quality of life.
Take the first step towards a pain-free future. Contact Integrated Physical Therapy & Wellness at 305.967.8976 to schedule your TMJ evaluation and treatment. Your journey to better jaw health starts now!


